Hierarchy of managing the runner: Part 1

By Michael Nitschke
Podiatrist
By John Osborne
Section Editor
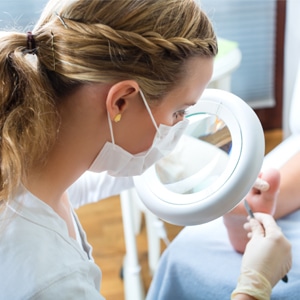
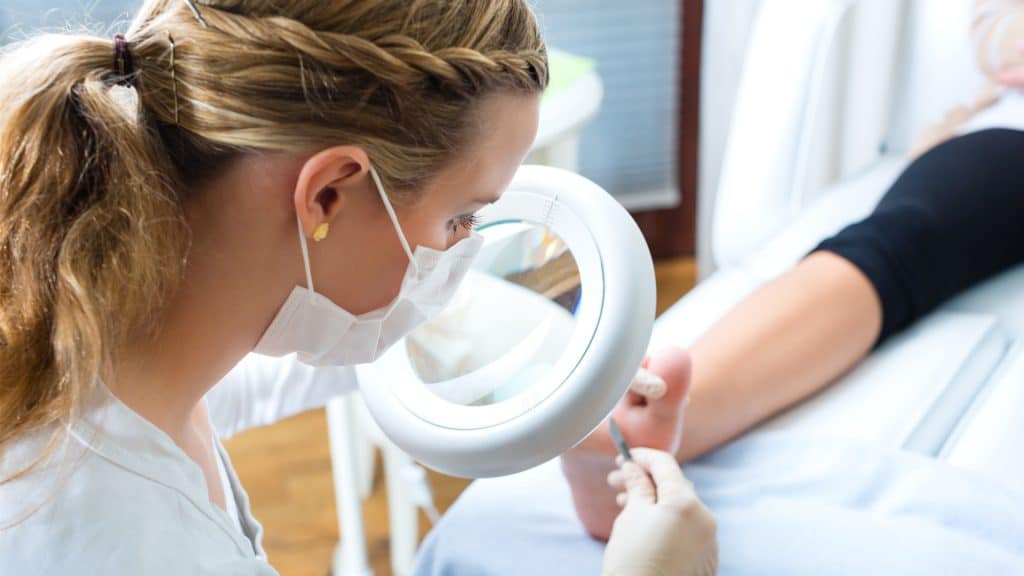
A common limitation to consistent training is running related injury (RRI), with incidence rates ranging between 2.5 to 33.0 injuries per 1000 hours of running exposure. When we consider the incidence of injury relative to running exposure, novice runners are more susceptible to RRI and 30 per cent of novice runners report quitting running within six months, with RRI cited as the main reason.
However, we still tend to see more injuries in sub-elite and elite runners as their training exposure is far greater. This important injury and/or illness is associated with not reaching their performance goals.
The truth behind RRI
What is the cause of RRI? Is it poor footwear? Is it poor running technique? Not enough stretching? These reasons are often perceived by runners as being the cause of RRI, yet it’s a lot broader than that. Despite RRI being multifactorial, it has been suggested that perhaps most RRI can be attributed to ‘training errors’.
Training errors up close
So, what’s a training error? A training error isn’t really defined clearly, but usually it’s something that leads to a disturbance of the balance between stress and rest (such as ‘too much too soon’). A training error that results in an RRI will more than likely require a complex system model to solve the problem, in order to create an optimal intervention. Very rarely is there an isolated risk factor, which means no ‘silver bullet’ solution exists to eliminate RRI.
If there was an isolated risk factor, incidence rates would have decreased by now, yet clearly they haven’t. To suggest an RRI can be prevented seems a bit far fetched perhaps, however we have knowledge of factors that increase risk. Unfortunately, knowing what may increase the risk of RRI does not necessarily protect individuals from getting injured. Humans may still make a training error despite knowing it is an error before making it.
A hierarchical approach
If it is helpful, I have found a hierarchical approach to triaging running related injuries to be of much use clinically (Figure 1).
Figure 1. Nitta’s hierarchy of sustainable running.
Simply put, one cannot sustain a running related injury without performing the act of running itself. If you buy a shoe that isn’t your ideal, or you have poor strength or flexibility and/or running biomechanics, these MAY increase your risk of a running injury, but you still need to run in order to get a RRI.
The above hierarchy of managing sustainable running was designed to prioritise which risk factors I clinically tend to see as the most important in order to reduce the risk of injury (that being, training characteristics [stress] + adaptation [rest]).
The hierarchy still places a focus on factors that may increase risk of injury, however, I don’t tend to consider these factors determining whether one will get injured, but perhaps more so WHAT structures may be at risk.
I also consider these are factors that can dictate the DOSAGE of running that one can handle (based on adaptation, tissue tolerance, biomechanics + equipment).
In summary
So after 22 years of physically running, and 15 years spent working with runners as a clinician (and now moving into practically coaching runners), my approach to working in this field has evolved. I consider my role as an educator who attempts to create a sustainable running model that reduces risk of injury or overtraining syndrome for the individual. Along the way, hopefully this will help to create a very self-efficacious runner who can maintain this with less assistance in the future.
Next month, Michael Nitschke continues this exploration further to focus on why prioritising the organisation of one’s training characteristics may be the most important consideration for consistent running. He also looks at the characteristics that cause injury, manipulation of loading to avoid injury, what sustainable training organisation looks like up close, and more.
AD
A proud STRIDE advertiser
The PhD – is it for me?
PhD degrees are considered ‘terminal degrees’, meaning that the recipient has achieved the highest formal degree in their field. Whilst this can bring significant credibility and enhance career prospects, it is not something that should be undertaken lightly, explains Dr Frances Henshaw.
Take a student on placement: it’s a great thing for all of us!

By Sarah Casey
Lecturer
Sarah Casey shares the benefits of student placements; for students, universities and clinicians.
Podiatry programs in Australia are expected to provide students with the opportunity to attend placements in a range of settings, including both public and private practices. Practitioners who offer a clinical placement opportunity to a student are providing the student with the opportunity to develop their skills in the workplace.
Benefits for students
This comes with a number of benefits:
- Students gain experience in the ‘real world’ outside university clinics, where appointments cannot take an hour or more, and where clinicians and patients sometimes have to juggle clinical considerations with financial and social constraints.
- Students get to experience different types of workplaces, in different locations. This can change (or confirm) a student’s career aspirations and planned geographical location.
Benefits for universities
Universities also see the benefits of students’ participation in placements outside the institution:
- External placement is an accreditation requirement – programs need placements to take on students in order for them to graduate.
- External placements can offer experiences and opportunities that students can’t achieve in the university’s own clinic.
Benefits for the profession
The podiatry profession also stand to benefit from the involvement of students in clinical practice placements:
- Currently, there is a shortage of podiatrists in Australia, particularly in rural and regional areas. As a profession, we need more podiatrists in order to maintain, and preferably increase the profile of our discipline. As podiatry programs move to increasing our scope of practice (particularly with regard to prescription of scheduled medicines), we need to ensure that we are the first port of call for any member of the public with a lower limb problem.
- Being able to provide students with a broad range of work and clinical experiences helps to develop the skills, attitudes and attributes of graduates. As the profession develops, it’s important that our workforce of the future understands the environment they are going to enter – complete with its challenges and strengths.
Benefits for clinicians
But what about clinicians – what do they get out of hosting a student on clinical placement?
- Hosting final year students, who can take on caseloads, can contribute to the productivity of the facility. It has been shown that taking students on placement can enhance productivity.
- Students can bring updated knowledge and theories, providing clinicians an opportunity to broaden and update their knowledge.
- Taking students on placement enhances opportunities for recruitment of graduates; directly by employing people who undertook student placement, and by promoting the reputation of your practice/department as a great place to work. This is especially advantageous to rural facilities that may experience difficulties in recruiting podiatrists. If you demonstrate that you are able to offer a graduate mentoring and opportunities that appeal to them, you are more likely to attract them to work in your practice when you need someone!
- Having students on placement provides a link with the university, introducing the possibility of research collaboration and research sharing. This link also ensures clinicians are kept informed of university seminars and professional development opportunities.
- Being involved in clinical education allows clinicians to be part of developing undergraduate curriculum and refining clinical education processes, e.g. participating in working groups and consultation processes.
- Students may contribute to their hosts’ professional development/CPD program. For example, final year students may work on special projects while on placement, that may not be possible otherwise. In addition, practitioners may choose to develop a program of activities for the student based on their stated placement objectives. This may involve a number of activities that contribute to the clinician’s professional development (and that can be recorded as such).
- Taking students on placement provides a valuable role in contributing to the profession of podiatry; we are a small discipline and it is important to ensure that we maintain the future supply of podiatry graduates ready to deliver the care the public need. If we can grow our profession, we have the potential to improve the standing and reputation of podiatry in the public eye.
- Being engaged with the placement process provides CPD opportunities, which is beneficial in terms of Ahpra registration as well as to our own development of skills and knowledge.
- Although there may be some costs associated with hosting a student on placement (for example, through having to slow down appointments), it represents a relatively low-cost way to engage in aspects of CPD that cannot be gained in other ways. From personal experience, I know that a really good way to bolster your own knowledge and practice is to teach someone else how to do what you do! It can also be a great way to remind yourself of where your strengths lie, and to identify where you could stand to improve (which feeds in to the CPD cycle).
A final note
It is important to acknowledge the concerns of practices who are considering taking students, particularly around the potential for a student to cause disruption and additional workload for placement hosts. Universities understand these concerns, and will work with hosts to reduce the likelihood of problems occurring, and to deal with any difficulties promptly if they arise. One of the most effective ways to minimise problems, in our experience, is to clearly set out expectations at the outset. Setting aside time on the first day or two for both parties to lay out what they need/would like to achieve from the placement can help to ensure that the placement goes smoothly, and that everyone benefits from the process.
Be part of the change in dementia
It is estimated that almost half a million Australians are affected by dementia and this figure is set to double in the next 25 years. Dr Kristy Robson explains why a greater awareness of this disease is needed, and how we can support people impacted by it. Dr Robson explains how this approach will lift the standard of care and hopefully reduce the rates of discrimination associated with this condition.
Meet Dr Kristy Robson

By Dr Fiona Hawke
Interviewer

By Dr Kristy Robson
Interviewee
What are you working on at the moment?
At the moment I am working with a team of researchers from Charles Sturt Uni and Bond Uni and we are undertaking 28 different rapid reviews on a range of occupational risk factors and the development of injuries for the Department of Veterans Affairs. I am also currently working on a manuscript focusing on how to design effective healthy ageing programs from the perspective of older people.
How could your research change clinical practice (now or in the future)?
I mainly research in the area of healthy ageing and injury risk and I am passionate about ensuring that research is not only translatable into clinical practice but also enables the voices of participants to be heard. I am a strong advocate for facilitating mixed method research approaches, where appropriate, so that clinicians can understand the impact of ageing or injuries, such as falls, from the older person’s perspective. This can often make research outcomes more meaningful and clinically relevant interventions more person-centred.
What first got you interested in research?
When I was in private practice, I had a number of very fit, active and contributing older members of the community have a fall. At one point I had three of these long-term clients all have a fall within one month. Two of them had to leave their homes and move into residential aged care and one passed away all because of their falls. This really sparked me into wanting to understand what the potential risk factors were for falls and as a clinician what could I be doing differently to try and minimise the harm of such falls. I went on to make this area the focus on my PhD.
How have things changed since then?
When I first started my PhD, I didn’t really have any experience in qualitative methods. The opportunity to talk to older people and their family members about their fall experiences was really enlightening. Qualitative methods are becoming a more common approach in research design that is seen as adding significant value to research. I have continued to actively research using qualitative methods particularly focusing on the lived experience of participants as this can be a very powerful narrative that can change the way we think about approaching healthcare.
Did/do you have a research mentor?
I have had a number of amazing experience researchers that have assisted me across my career and I continue to do research with them now on different projects. Starting out in research can be very daunting and overwhelming, so it is important to have good people around you to support you but also challenge your thinking along your journey. Having a good team around you whether it is a specific mentor, or a research group of likeminded people is always a useful strategy to bounce ideas off.
What are the best parts of being a researcher?
I think the best part of being a researcher is the ability to think critically about a problem and contribute to solutions to make the problem better. I also love the ability to work with lots of diverse people and as a qualitative researcher the ability to bring participants’ experiences to life is the best part of my job.
What are the most challenging parts of being a researcher?
Like any researcher the most challenging aspects are time and money. There never seems to be enough time to do the projects you want, and grant funding is a scarce commodity.
What advice would you give a clinical podiatrist wanting to get involved in research?
The best advice is to start with a conversation. If you have a topic of interest then do some reading on who is publishing in the area and reach out to them and have a chat. If you are interested in just developing your research skills, then reaching out to a local university to see what opportunities might exist to co-supervise an honours student is a really great way to introduce yourself to the world of research in a supportive environment.
What keeps you going outside of podiatry?
I am a creative person, so I love to make things. I also love to travel so I’m looking forward to the day when that’s back on the agenda again!
If you weren’t a podiatrist/researcher, what would you be?
I was recently introduced to the world of cybersecurity and I have found it fascinating (and a little bit scary). I think if I had to pivot in a new direction, I would become a cybersecurity analyst because I love solving problems.
Where do you think your research interests will lead you next?
I try to keep an open mind to possibilities so not sure what the next direction will be.
Auditing foot & ankle surgery to improve outcomes: The ACPS experience
Dr Rob Hermann reflects on the development and implementation of an online audit tool to measure and report foot and ankle surgical outcomes, and in doing so, he advocates the importance of surgical audits.
Cultural safety in our professional capabilities

By James Gerrard
Section Editor
At the time of writing this in October 2021, recent weeks have seen the release of our profession’s new professional capabilities, which were published in September on the Podiatry Board of Australia’s website.
The Board completed a drafting and public consultation process of our new professional capabilities, which led to their release and imminent instatement. Our new professional capabilities will come into effect on 1 January 2022.
The ‘professional capabilities’ for both podiatrists and podiatric surgeons are available here.
Here are some key points regarding the thresholds that registered podiatrists will need to meet and maintain within our newly released professional capabilities relating to cultural safety:
- Being a professional and ethical practitioner: ‘Treat each patient with respect, dignity and care.’ This is enabled by displaying culturally safe practice and recognising and respecting ‘Aboriginal and Torres Strait Islander Peoples’ ways of knowing, being and doing in the context of history, culture and diversity.’
- Being a communicator and collaborator: ‘Examine and reflect on how one’s own culture influences perceptions and interactions with others from different cultures.’ The document lists enabling components for registered podiatrists be able to continually develop this capability. These are:
- ‘understand the impact of systemic racism and recognise the influence of one’s own cultural identity on perceptions of and interactions with Aboriginal and Torres Strait Islander Peoples and people from other cultures’
- ‘recognise different forms of cultural bias and associated stereotypes that impact on Aboriginal and Torres Strait Islander health; and practice in a culturally sensitive and inclusive manner’
- ‘recognise the role of history and relationships between Aboriginal and Torres Strait Islander Peoples and white Australian society and how this has affected the inequitable distribution of privileges’
These professional capabilities provide a pathway for our individual and collective development of cultural safety and for the ongoing development of cultural safety as a fundamental skill of a podiatrist.
Next steps
As we continue our pursuit of the Ahpra strategy to embed cultural safety into the health system, these new professional capabilities will add to our profession’s key achievements.
These include recommending and advocating for changes to the Health Practitioner Regulation National Law to ensure consistency in cultural safety for Aboriginal and Torres Strait Islander people.
We are signatories to the National Scheme’s strategy developed with the leadership of Aboriginal and Torres Strait Islander health organisations and individuals and, through the Podiatry Board of Australia, also proudly endorse it, see here.
All registered podiatrists across all settings are encouraged to thoroughly read over the ‘Approval of new professional capabilities for podiatrists and podiatric surgeons’ released under the umbrella of The National Scheme – available here with excerpts below.
‘At its July 2021 meeting, the Board approved new professional capabilities for podiatrists and podiatric surgeons. They will come into effect 1 January 2022.
The professional capabilities identify the knowledge, skills and professional attributes needed to safely and competently practice as a podiatrist or podiatric surgeon in Australia. They describe the threshold or minimum level of professional capability needed for registration as a podiatrist or podiatric surgeon.
The Podiatry Accreditation Committee developed the new professional capabilities for the Board, which included consulting widely with the profession and other stakeholders.
The new professional capabilities reflect contemporary podiatry and podiatric surgery practice in Australia. They are founded on person-centred, evidenced-based practice, and make cultural safety a key component of safe care, particularly with respect to Aboriginal and Torres Strait Islander Peoples.
The professional capabilities will be used by the Board as a reference point for threshold capability when exercising its statutory functions.
The new professional capabilities will be published on the Board’s website in early September 2021, together with supporting information such as FAQs.’
Inducting new employees
New employees, new start – it can be incredibly overwhelming for new employees to begin employment in a completely new workplace, whether it be their first job upon graduation, or their tenth. It is in the employer’s best interest to be able to facilitate their transition into the workplace as smoothly as possible, and this is best done through an induction process.
People with knee osteoarthritis have pronated feet
Knee osteoarthritis (KOA) is a common condition characterized by chronic joint pain and stiffness, leading to the limitation of daily living activities and physical function. Foot characteristics and mechanics, including static foot posture and dynamic foot function may significantly contribute to musculoskeletal conditions of the lower limb. Therefore the aim of this systematic review was to provide an overview of the foot characteristics and mechanics that have been evaluated in the literature in people with KOA, and investigate whether foot characteristics and mechanics vary between people with and without KOA.
Article
Five electronic databases were searched for studies including the terms ‘foot’ and ‘knee osteoarthritis’. A total of 10,899 studies were retrieved and after review of the literature, 39 articles found to have evaluated foot characteristics and/or mechanics in individuals with KOA.
The studies
The 39 included studies included a total of 2260 participants, and of the studies 25 were observational studies and 14 were intervention studies. The majority of studies (64%) were categorised as low study quality using the STROBE checklist.
The results
Two measures, foot progression ankle and peak rearfoot eversion angle were reported in a way allowed for combined analysis of data through meta-analysis. These results indicated no significant difference between people with and without KOA. Foot posture was reported differently in six different studies, making meta-analysis not possible. However, the studies indicated more pronated foot posture in people with KOA compared to people without. As the measurement of foot posture occurred at a single point in time, it is not possible to determine whether foot posture was a cause or effect of KOA. However, the findings highlight the importance of the kinetic chain and biomechanical influence of one joint on another.
The limitations
There were limitations with the systematic review. Foot measures were only reported in one or two studies with a small sample of participants, which may limit their generalisability to the wider KOA population. Further, it was identified that the quality of the studies were mostly low.
The conclusion
Overall, this systematic review provided a useful snapshot of our current understanding of the link between the foot and KOA.
You can read the full study here.
What to do in the event of a cyber attack: Part 1

By Natalie Policki
National Membership Manager
Many of us have been on the receiving end of spam calls from the ‘tax office’ or perhaps been the recipient of fake text messages advising us that our ‘parcel is ready for collection’. We know all too well that one false click can lead to a virus. But let’s go further and reflect on the clinic or practice you work at. What would your team do in the event of a cyber attack?
Notify those who need to know
The all important starting point is to notify those who need to know. You must notify your clients if your system is hacked, attacked or compromised in any way. If you don’t do this, you risk facing significant fines for non-compliance. The general idea behind this zero-tolerance approach is that once your clients are notified it empowers them to take necessary steps to protect their identity. Whereas if you don’t tell them, you restrict their opportunity to take these steps.
Be responsive
Timing is crucial. The longer you wait, the higher the likelihood that your clients may learn about this attack from another source, which can really damage your clinic’s reputation.
This all falls within the broader context of the Notifiable Data Breaches Scheme (NBD), which came into effect on 22 February 2018 and it pays to be familiar with this scheme. As previously stated, its rules apply to all agencies and organisations that are covered by the Australian Privacy Act 1988 (Cth). Regardless of turnover, the Privacy Act covers any business that is:
- a health service provider
- trading in personal information
- a contractor that provides services under a Commonwealth contract
- an operator of a residential tenancy database
- a credit reporting body.
What the NDB says
When a data breach occurs, the NDB states that your priority as a business is to contain the breach and take remedial action. If your corrective action fails to mitigate the risk of serious harm, you must notify the Commissioner and the affected individuals.
Did you know?
Healthcare businesses are valuable targets because they hold sensitive personal information and credit card details – worth up to four times more to a cyber criminal than a simple ransom demand. In 2019, Australia’s health sector accounted for 22 per cent of all data breaches, making it the highest reporting sector in the country.
Steps you can take
So with all that in mind, here’s what you can do in the event of a cyber attack. As always, please seek professional advice in the event this happens to you.
- The Office of the Australian Information Commissioner (OAIC) has an online form that can be used to prepare a statement to the Commissioner about the breach.
- When notifying clients, you can stick to your standard form of communication whether it be a letter, email, phone or online. The notification must include the type of breach, the personal information affected and advice about what they should do. Other tips you may want to include are to:
- Advise clients on what steps to take to remediate their affected identity or protect themselves. Offer avenues of support, such as a helpline or a micro-website.
- Ensure your client communication contains contact details of credit reporting bodies such as Equifax so they can put an alert or ban on their credit file.
- Consider guiding clients towards credit monitoring plans such as Your Credit & Identity which can give clients an early heads up on potential identity theft.
- Provide clients with the details of an identity remediation partner. For example, IDCARE is a not-for-profit charity who can work with your clients to go through any necessary mitigation steps.
- Prepare your staff on how to field client questions about the breach. Bear in mind that your clients may be significantly inconvenienced by this breach so ensure your team is responsive to their frustrations and empathises with the potential time and effort involved on your client’s part.
Next month: We look at the three criteria behind when a data breach is notifiable, what is considered ‘personal information’, and who is responsible if you’re using a third party.
Additional resources
- BMS Group’s Cyber Liability Insurance can be purchased alongside your membership. For example, after an attack, Cyber Insurance will cover the following costs:
- Third party claims against you
- Business interruption and costs to restore your data
- Notifying your customers and employees of the breach.
- Contact BMS via phone or email to learn more about Cyber Liability Insurance: podiatry@bmsgroup.com | 1800 514 933 or proceed to the online purchase process, found here.
- Australian Government’s STAY SMART ONLINE has tools on how to protect your business and free alerts.
- Digital health agency offers cyber security training and resources to directly assist healthcare providers.
- Equifax’s has a range of credit and identity products.
- Our website contains useful tips and insights.