APodA advocacy update
- 560 Words
- 4 minutes reading time

By Cindy Laird
Advocacy Manager
The Scope of Practice outline is now available for podiatrists to download. Advocacy Manager, Cindy Laird, shares the details.
Scope of Practice update
One of our key strategic priorities was to develop a Scope of Practice outline for the podiatry profession. There was a need to provide a clearer definition of the scope of practice for podiatrists and for the benefit of health consumers, other health professionals, and statutory authorities.
The goal
Our purpose was to provide information on the expanded scope of the podiatry profession. And so it is purposefully written in general terms as to not risk defining ‘practice’ too narrowly.
The process
The drafting process itself was comprehensive, with evidence to inform the document being gathered from the profession and overseen by the APodA Advocacy Committee. Feedback was also sought from the profession, our membership, the APodA Regional Committees, external consumer feedback and the Consumers Health Forum of Australia.
The result
The Scope of Practice outline provides a contemporary reflection of the podiatry profession in Australia. Included in the document is the definition of podiatry, practice areas and settings, anatomical considerations and qualifications.
The impact
This document will be used to:
- Advance the podiatry profession
- Benefit the consumer
- Benefit podiatrists
- Benefit the profession, and;
- Encourage efficiencies with the health system.
As a member of the APodA, you can use this document in your own promotion amongst other health professionals and the community.
Thank you
Thank you to everyone who was involved in developing this important outline. It was a collaborative process and we should be proud of the progress made to date.
Questions?
If you have any questions about this issue please contact our Advocacy Manager, Cindy Laird at cindy.laird@podiatry.org.au
After two years, the ‘Royal Commission into Aged Care Quality and Safety’ has handed down its final report and recommendations, which includes an extensive plan to overhaul Australia’s aged care system. Advocacy Manager, Cindy Laird explains how these findings shape podiatry guidelines.
Aged care update
To be honest, much of this report makes for sobering reading. In addressing the current system to the Commission, serious inadequacies are noted when it comes to providing even the most basic care for older Australians.
Online resources
You can also read the official findings by the Royal Commission and we have summarised the key findings that link into allied health and podiatry guidelines. Below is an excerpt from this summary.
“Our goal is that all older Australians can maintain dignity and quality of life while being cared for within the aged care system.
Our Podiatry guidelines in residential aged care homes have been developed as the standards we expect when delivering services in residential aged care facilities. The guidelines have been sent to residential aged care homes in Australia.
Many of the Royal Commission’s findings align with the APodA’s recommendations for minimum standards for podiatry in residential aged care facilities. We will be surveying RACFs later this year to measure the impact both the Commission’s report and recommendations – and our guidelines – have had on the quality of allied health and podiatry services in aged care.”
More information
Head here for more background on this issue.
Update on the regulatory changes at the Therapeutics Goods Administration (TGA)
- 850 Words
- 7 minutes reading time
A lot of questions have been sparked by regulatory changes at the Therapeutics Goods Administration (TGA) regarding the supply of personalised medical devices (including orthotics). Advocacy Manager, Cindy Laird, addresses these issues.
Launching our Indigenous section: Meet the section editor
- 560 Words
- 5 minutes reading time

By James Gerrard
Section Editor
Welcome James! Why do you feel podiatrists will benefit from reading this section, regardless of whether they are directly involved in Indigenous issues or not?
There is so much fantastic work being done in this space that doesn’t always translate into research published within the Western academy. This section in STRIDE is a means of promoting such work so that podiatry can benefit from the combined knowledge of two worldviews to progress our profession towards improved and safer care. Podiatrists reading this section of STRIDE will learn so much from First Nations Peoples and those who live with, and work closely with, Aboriginal and Torres Strait Islander Peoples. The benefit to all of us is that the principles of cultural safety are applicable to all cultural backgrounds; promoting inclusion of diversity in religion, sexuality, ethnicity and more.
Why do you feel strongly about creating a section in STRIDE which is dedicated to Aboriginal and Torres Strait Islander Peoples, and related issues and topics?
I am thrilled to have the opportunity to help introduce and to work within this new section of STRIDE magazine.
This section will be devoted to Aboriginal and Torres Strait Islander Peoples, their cultures, First Nations foot health, and Aboriginal and Torres Strait Islander worldviews, ways of knowing, ways of being and ways of doing. I feel so strongly about being involved in this section of STRIDE. When learning with, and from, Aboriginal and Torres Strait Islander Peoples we (as well-intentioned podiatrists) can develop skillsets that result in actions that change practice and systems, and promote health outcome equity.
Who do you see being involved in the creation of this section and why is their involvement key here?
As section editor of this section, I will work with First Nations authorship and input to bring Aboriginal and Torres Strait Islander voices to all STRIDE issues. This is key because the experts in Aboriginal and Torres Strait Islander health are, of course, Aboriginal and Torres Strait Islander Peoples.
Okay, now tell us some more about yourself?
I consider myself an average Australian podiatrist. Currently, I am a podiatry PhD candidate at the University of Newcastle and a lecturer at La Trobe University within the discipline of podiatry. I am currently very lucky to be involved in research with First Nations Peoples that develops mutually beneficial relationships, fosters reciprocity, advocates self-determination, and delivers results that benefit communities.
What themes would you like to discuss over the coming months?
I am excited about covering a lot of themes, not just in the coming months, but beyond that as well. Topics such as self-reflection, unconscious bias, racism and self-determination will hopefully spark impetus for improvements in a lot of us across Country; but presenting First Nations lived experiences and expert opinions relevant to podiatry clinical practice, education and research will definitely be covered too.
Anything else to add?
I would love to add that anyone can contact me at any time regarding wanting to contribute within this space, or on topics they would like to learn more about. I’m at J.Gerrard@latrobe.edu.au
The role of podiatry in sports medicine
Certified Sports Podiatrist John Osborne facilitates a debrief with three professionals in the sporting world. They open up about their experiences of podiatry and podiatrists, as well as their expectations of the profession.
Clinical technology in practice
Alongside new developments, when it comes to our understanding of the lower limb and its problems, an ever-growing number of gadgets can be used to help assess and treat patients. Section editor Andrew Schox explains how we might choose, use and review these technologies in clinical practice.
Ageing: its stereotypes and its impact
- 1270 Words
- 8 minutes reading time
What role do podiatrists have in shaping the conversation around ageing and its stereotypes? Assoc Prof Caroline Robinson explores this issue.
The role of visual signs – are they reliable in peripheral arterial disease (PAD) screening?
World Health Day is taking place this month on April 7th with the theme of building a fairer, healthier world. This month's cardiovascular section is focusing on an aspect of evidence-based practice for peripheral vascular assessment for improved clinical decision-making and preventative care.
Understanding personality types can help you to understand how you best learn, so let’s dive into the well known Myers-Briggs profiles. Known officially as the Myers-Briggs Type Indicator (MBTI) these 16 different personality types cover a range of personality traits, from ‘thinking’ to ‘feeling’, from ‘introvert’ to ‘extrovert’, and so on.
Test your personality profile
If you want to run the test on yourself for free (or on your family and friends!) there are a range of online platforms available. Once you have taken the test, consider then reflecting on how your personality profile can help you to get the most out of your Continuing Professional Development (CPD) activities. For example, the different categories for each personality profile range from being seen as ‘The Helper’ (ESFJ) to ‘The Doer’ (ESTP) or ‘The Performer’ (ESFP). Perhaps reflect on the defined strengths and weaknesses of your profile to discover how you can bring that into your approach for learning?
Get to know you
If you benefit from that experience, consider doing some more ‘career-focussed’ tests, still within the scope of MBTI. These online tests require paid access but they test a range of career issues; from whether you may be close to experiencing burnout or what your career values are through to discovering what kind of leadership style you have and even exploring what motivates you at work to want to succeed.
Happy exploring!
- 280 Words
- 2 minutes reading time

By Annette Harris
CPD Manager
Considered gaining endorsement?
- 590 Words
- 4 minutes reading time

By Tom Walsh
Lecturer and Researcher
Have you considered becoming an endorsed prescriber? Dr Tom Walsh explains the process and shares some surprising insights along the way.
As the Podiatry Accreditation Committee homes in on finalising accreditation standards, some universities are preparing curricula to train students and practising podiatrists to gain endorsement for scheduled medicines. The number of podiatrists with endorsement is therefore likely to rise, perhaps swiftly, over the next decade.
What endorsement acknowledges
Endorsement of registration with the Podiatry Board of Australia for scheduled medicines acknowledges that a practitioner has the relevant skills and training to administer, obtain, possess, prescribe, sell, supply and use Schedule 2, 3, 4 or 8 medicines on the national formulary. While the regulations as to what practitioners are allowed to do still rests with each state, most states green light the full range of medicines on the formulary.
The process for prescribing
The recommended process for prescribing has been well-described and follows four stages.
- Information gathering
- Clinical decision-making
- Communicating the decision, and;
- Monitoring and review
These stages are clearly not specific to prescribing and indeed would be used by most clinicians no matter who they are consulting and what they are implementing.
A word of caution
With prescribing in your armamentarium, there is however a need to be ultra-vigilant with history taking, as to avoid providing a patient with a medicine that interacts with something that they currently take or that may not be suitable with an underlying condition. If you do determine that a medicine could be useful, you must then consider whether the benefit(s) of the medicine outweigh the potential harm(s). This is something that you and the patient both need to consider.
Medical side effects on impact and the foot and ankle
One of the most insightful aspects of the endorsement training was understanding how many medicines have adverse effects that may manifest as foot/ankle complaints. Over 200 medicines used in Australia have adverse effects including arthralgia, myalgia, myopathy, onycholysis, paraesthesia, paronychia, peripheral neuropathy, synovitis and tendinopathy. Many are repeat offenders. One may even cause plantar fibromatoses!
The beauty of using medicines for treatment is that medicines undergo rigorous testing even before they get to clinical trials, their usefulness and potential for adverse effects are well documented and constantly updated. The scale of the research (and ongoing safety and effectiveness data) used for these therapies is almost unlike any other treatment a podiatrist can provide.
An investigative process
Given scheduled medicines are so heavily tested, and given the standardisation of the drug components, you can determine the actual therapeutic effect of the medicine, and tease out what is likely due to placebo, natural history or other non-intervention related mechanisms. The use of scheduled medicines in our undergraduate and postgraduate student clinics is rewarding for both the student and patient. The resolution of either an infected ingrown toenail with a short course of antibiotics, or relief of a painful joint with a corticosteroid can be quick, cheap, and satisfying.
Up to you
If you have an interest in broadening your scope of practice using regulated and proven therapies, then endorsement for scheduled medicines may be something to consider. An accredited university can provide undergraduate and postgraduate students with the resources required to successfully complete Pathway A – some may be able to offer this as early as 2022.
Professor Karl Landorf steps down as trustee of APERF
- 690 Words
- 6 minutes reading time

By Professor Hylton Menz
Trustee, APERF
 What attracted you to joining APERF as a trustee?
What attracted you to joining APERF as a trustee?
I was attracted to joining APERF as trustee because I was a recipient of an APERF grant in 1999 to conduct a trial of foot orthoses for plantar heel pain. Through this experience I could appreciate how critical APERF was in supporting foot and ankle researchers – both experienced researchers conducting cutting edge research, as well as inexperienced researchers just starting out. I cannot emphasise this last point enough; APERF has really helped many inexperienced researchers start their research careers, some of whom have moved into highly influential positions that have greatly helped the podiatry profession.
What did you find the most enjoyable aspects of being a trustee and chair of APERF?
There were three main aspects that were most enjoyable – the positive reaction from applicants when they received a grant, working with the other trustees, who all have tremendous research experience and are highly ethical and caring individuals, and the very kind and selfless individuals in our profession that have donated to or raised money for APERF.
What is the biggest challenge facing APERF?
The biggest challenge by far is the ongoing need for a consistent and healthy funding source to be able to offer grants. Donations are one of the greatest sources of funds, so I encourage those who do donate to keep doing so, and those that don’t, please consider setting up a regular donation to help support APERF funding further research into projects that directly relate to podiatric practice.
Dr Shan Bergin has now taken over the role of chair of APERF. What different skills do you think she brings to the role?
Shan has many great skills and she has the drive to keep APERF moving forward – she is an ideal person to be chair of APERF. Shan is a no-nonsense type of person, which I really admire, and I am impressed with how she just gets on with the job. Importantly, Shan comes from a broader public health background compared to me, so I think this difference will benefit APERF.
Any final reflections or comments?
Yes! Firstly, a big thank you to all podiatrists who have supported APERF over the last three decades (both financial and in-kind support). I cannot thank you enough. Without this support, our profession would not have produced so many studies. The impact of these studies on foot health is irrefutable. This support has brought substantial benefits to people with foot problems. Further, the studies produced from APERF grants have benefited the profession substantially. These studies have contributed to the evidence base of podiatry, which has placed us well by positioning podiatry as a mainstream evidence-based profession that is viewed favourably by the government and other key health institutions. The profession in Australia should be very proud of APERF and how it has contributed to the standing of the profession.
The Australian Podiatry Association and current trustees would like to sincerely thank Professor Landorf for his dedicated service to the profession through his contribution to and leadership of APERF over the past 15 years.
The Australian Podiatry Education and Research Foundation (APERF) was established in 1991 and exists to advance research into the causes, prevention, and treatment of foot problems. APERF is a charitable trust that is currently overseen by seven trustees. Since its establishment, APERF has supported 81 research projects and has awarded $495,000 in research grants. For more information about APERF or to make a donation, please visit the website and follow on Twitter @_aperf
Early in my podiatry career, whilst undertaking a locum community health service role, I was confronted with a dilemma. A child I was consulting needed orthotic devices to manage their foot pain, however, their parents were unable to afford the expense. I liaised with my line manager who consented for the organisation to provide the devices pro bono. However, in a subsequent meeting, the senior manager disapproved of this action. The dilemma created an intriguing discussion about roles, responsibilities and the appropriate course of action for all parties.
The costs involved
In public hospitals and community health centres it is generally expected that the parents or guardians of children who are prescribed orthotic devices will cover the expenses associated with the direct manufacture of devices. These costs are significantly less than orthotic devices purchased in a private setting, yet the monetary outlay may still prove considerable.
When you consider families that are experiencing financial disadvantage and then you factor in the constant growth of any child’s feet, new and larger devices may need to be purchased fairly often.
Alternate pathways
There are alternate pathways available for podiatrists to dispense orthotic devices to children of financially disadvantaged households who are unable to afford associated costs.
For example, podiatrists practising in Victorian public hospitals and community health centres are somewhat familiar with the Department of Health and Human Services’ Victorian Aids and Equipment Program. This program provides people experiencing a permanent or long-term disability with access to subsidised aids equipment, home and vehicle modifications. EnableNSW is the equivalent platform for NSW-based podiatrists to assist local people with health needs. If you know of similar programs that are active in other states, please let me know and I can update this.
The goal behind Footscape
Upon establishing Footscape I was determined that our podiatry charity could provide an effective pathway to fund orthotic devices for disadvantaged children in a timely manner.
Indeed, I’m proud to report that since 2013 the Children’s Orthotic Project has funded three hundred orthotic devices for Victorian children encountering foot pathology attending affiliate organisations. In addition, during the past two years, recipient children are concurrently eligible to receive new footwear to aid their schooling and recreation. Footscape has welcomed the amazing support of Orthotech Laboratory to ensure the sustainability of the Children’s Orthotic Project.
Sonia Lancaster, podiatrist at Sunraysia Community Health Services, highlighted the benefits of the project to the Mildura region:
‘Since 2018 the Footscape Children’s Orthotic Project has enabled Sunraysia Community Health Services to fast-track provision of orthotics and footwear to eligible children who otherwise would struggle to afford. We have forged closer links with the wider multidisciplinary team, having a number of referrals from within Sunraysia Community Health Services and externally from private podiatrists.’
Our future plans
The Footscape team are now endeavouring to streamline and expand this project throughout Australia. Podiatrists employed in public hospitals and community health centres across the country and encouraged to liaise with Footscape and get involved with delivering the Children’s Orthotic Project to assist financially disadvantaged children encountering foot pathology.
Reach out
Please contact me anytime to get involved or find out more.
- 560 Words
- 4 minutes reading time

By Anthony Lewis
CEO, Footscape
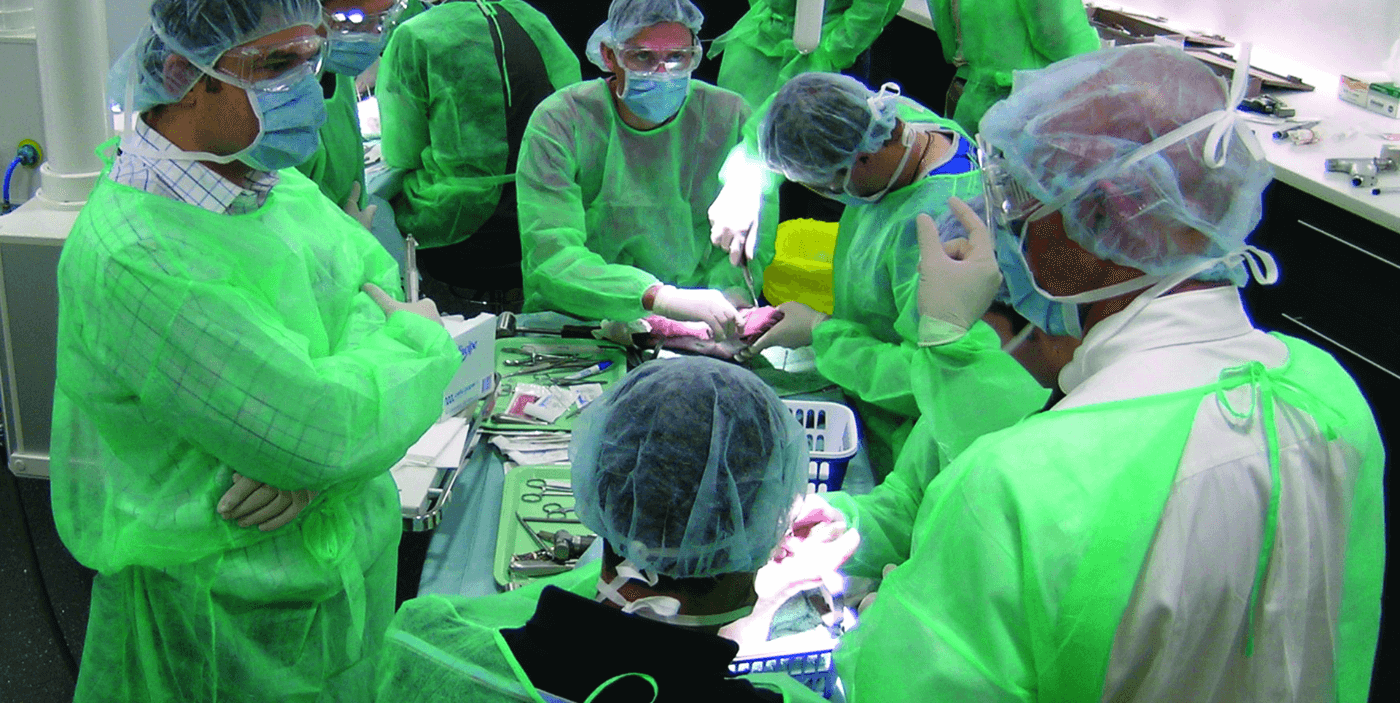
The history of podiatric surgery in Australia: Part 1
The birth of podiatric surgery was inspired by podiatrists who worked hard to see this chapter begin in Australia. Here’s the backstory on how it came to be.
Without a doubt, you are aware of the TGA’s announcement regarding customised orthotics falling under the new category of patient-matched devices. Despite being a biomedical engineer and not a podiatrist, I am still fortunate enough to be included in numerous podiatry Facebook groups where I have seen the reaction to this announcement unfold.
With a medical device commercialisation background, I have been asked to help distil what this announcement means for you and how this can benefit you, your clinic and the overall podiatry profession.
What we know
Orthotics are medical devices. Suppose you get a chance to review the Therapeutic Goods Act 1989. You would find that the definition of medical devices includes products intending to treat or alleviate injury or modify the body’s anatomical or physiological functions. Fortunately, orthotics don’t have a measuring function, are not provided sterile, don’t connect to an energy source and are non-invasive. This means that they generally fall under a ‘class 1 medical device’. The TGA has an excellent tool for you to use, which you can access here.
Who is the manufacturer?
But, who is the manufacturer? This question was the most common one I saw in those Facebook groups. If you are involved in the design, production, packaging or labelling of the device, you will find you are a manufacturer. It seems to me, the confusion behind this statement surrounds whether or not you are involved in the ‘design’ or ‘production’.
Firstly, ask yourself, ‘do you believe you are designing the orthotic or sizing up the patient?’ Suppose you’re working with an orthotic laboratory that has provided you with a framework to measure a patient, or you are assembling or adapting the device for an individual patient without affecting the intended purpose. In that case, you are not designing the device. You are likely not a manufacturer. If you are following your processes, not operating with a framework supplied to you by the laboratory, and/or you are defining the orthotic’s intended use, you may inadvertently be designing the orthotic! Similarly, if you are producing the orthotics entirely in-house, you are quite clearly the manufacturer.
Change can be scary, but in this case, there are plenty of potential benefits. While the TGA will now expect a higher version of quality control to be placed on orthotics, this means you will be able to communicate higher-quality goods to your patients. Because you will have to verify that you are sourcing safe materials through documentation, you can now ensure your suppliers are providing safe materials for your clinic. Have you ever seen proof of that?
A word for clinic owners
And lastly, for the owners of clinics. If you have multiple podiatrists manufacturing orthotics on-site, you should develop and document procedures for assessing patients, designing the orthotic, and verifying the patient’s orthotics. This will allow you to ensure graduate and junior podiatrists are prescribing within your established framework and have the design decisions made by a previous podiatrist who might have since left the clinic.
Good luck!
You can contact Ben via ben@solushin.com or on LinkedIn.

By Ben Lindsay – section editor
Podiatrist, software developer, technologist and futurist.
Long-term casuals: What you need to know
- 1000 Words
- 7 minutes reading time

By Joseph McHardy
APodA HR Advisory Service
The issue of employing long-term casuals has become increasingly prominent in Australian workplaces in recent years, with award specific obligations introduced for employers and employees in 2018 to address the associated complexities. Here’s the low-down on what you need to know.
The complexities of long-term casual employment translates to ongoing difficulties in the Australian industrial relations landscape. At the time of writing, legislation is being debated in parliament to introduce sweeping reforms via the Fair Work Amendment (Supporting Australia’s Jobs and Economic Recovery) Bill 2020.
One of the primary aims of this bill is to ensure that all parties e.g. employers, employees, employer and employee associations and so forth, have a clear and concise understanding of the legal definition of casual employment and corresponding conditions.
How does this affect you?
Given the significance of this issue, the team at the APodA HR Advisory Service thought it pertinent to remind members of their existing obligations in the Health Professionals and Support Services Award 2020 (“HPSSA”). This award applies to the majority – if not all – employers and employees in private practice in Australia.*
*Excludes unincorporated entities in WA.
What is a casual employee?
First up, let’s revisit the definition of a casual employee. As per the HPSSA, a casual employee is engaged on an hourly basis rather than as a part-time, full-time or fixed-term employee. They can be engaged to work up to and including 38 ordinary hours per week – with a minimum engagement period of three hours. The most recognisable attribute that distinguishes casual employees is the 25% loading they receive – which is intended to compensate them in lieu of the paid leave entitlements of permanent employees.
Although not explicitly enshrined in law, it is commonly understood that casual employees are engaged on an as-needs basis and shouldn’t have any guarantee nor expectation of ongoing work. This is implied by the reference to casual employees being engaged on an ‘hourly basis’.
What has made this issue prominent?
Complications have arisen in recent years for those employees who are engaged as casuals but work for their employers according to a regular pattern (and have done so for some time).
There has been an increasing opinion that these types of engagements do not align with the true nature of casual employment and that, in some cases, employers have been engaging individuals in this way to avoid paying leave entitlements and to make terminations easier.
In fact, there have been several recent high-profile cases – namely WorkPac v Skene (2018) and WorkPac v Rossato (2020) – where the courts assessed the relationship between employer and employee and determined that the individuals were not truly casual employees, despite their contracts saying so.
This resulted in adverse outcomes for these employers and sparked concerns amongst employers and employer associations that legal precedent is being set.
As with any legal proceedings, an important factor influencing the court’s decision is the individual circumstances at play. For this reason, it is critical employers in the podiatry profession understand these particular cases do not necessarily dictate what would happen if their business were to encounter a similar problem.
That said, it is important for employers to consider how these decisions may impact their casual workforce and make decisions if/as required.
Existing obligations to be aware of
The HPSSA allows regular casuals to request their employment be converted to permanent employment. A regular casual is defined as one who has worked a consistent pattern of hours which, without significant adjustment, they could continue to do as a permanent.
Whether or not they can convert to full-time or part-time employment will depend on the number of weekly hours they have regularly been working as a casual.
A practical solution to a challenge
A difficult question has arisen regarding long-term casuals who don’t wish to convert to permanency. Although the desire to remain casual is theirs, this cannot guarantee there may not be risks for employers later.
For this reason, the APodA HR Advisory Service recommends two key strategies to mitigate risk:
- Periodically offer the opportunity to convert to permanency in writing (ideally, every 12 months), and;
- List the 25% casual loading as a separate item on their payslip.
These two actions will protect an employer insofar as reasonably practicable from future risk. For instance, if a casual alleged they should have been treated as permanent and demanded leave entitlements retrospectively, these actions could act as part of an employer’s defence they have complied with the law by:
- Clarifying the intention of both parties with regard to the employee’s employment status, and;
- Compensated the employee financially with the casual loading
It is important we highlight that we cannot confirm how courts and/or industrial tribunals would view these actions. For example, we cannot guarantee they would entirely mitigate risk. However, we believe these to be the best tools given our current framework.
Looking to the future
The legislation currently before Parliament is seeking to insert a tighter definition of casual employment into the Fair Work Act as well as casual conversion provisions for award-free employees as well as award-covered employees.
As the situation progresses, the team at the APodA HR Advisory Service will ensure members are kept in the loop. Until then, we recommend employers review their current arrangements with casual employees in line with the information given here.
Disclaimer
The material contained in this publication is general comment and is not intended as advice on any particular matter. No reader should act or fail to act on the basis of any material contained herein. The material contained in this publication should not be relied on as a substitute for legal or professional advice on any particular matter. Wentworth Advantage Pty Ltd, expressly disclaim all and any liability to any persons whatsoever in respect of anything done or omitted to be done by any such person in reliance whether in whole or in part upon any of the contents of this publication. Without limiting the generality of this disclaimer, no author or editor shall have any responsibility for any other author or editor. For further information please contact Wentworth Advantage Pty Ltd.
©Wentworth Advantage Pty Ltd 2020

By Steph Cooper
How COVID impacted on homelessness + foot health
- 600 Words
- 5 minutes reading time

By Andrew Barlow
Founding Member, QLD Orthotics

By Tom Brough
Founding Member, QLD Orthotics
Many challenges affect people who experience homelessness, and while COVID certainly brought its share of setbacks, it also brought some interesting developments on the health front.
The sobering news
How long did rough sleepers go without podiatric care during COVID? Approximately between March 2020 to August 2020. That’s around half a year spent experiencing the following additional challenges.
- Most homeless shelters were shut or reduced to limited services during COVID, and;
- Allied health services were often not provided on a volunteer basis, due to strict COVID safe measures. Though GP and some specific charity organisations allied health care access were provided during this time.

What might have happened if we had not been able to do this? There might have been a regression in conditions due to the lack of podiatry care; whether related to wounds, musculoskeletal conditions, dermatological conditions or a range of other conditions.
In fact, some people who experienced homelessness ended up in hospital with foot infections due to lack of treatment, made worse by the strain on the public hospital system from COVID. This is not good enough, and yet when a pandemic such as COVID hits, there are so many variables that need to be considered and weighed up.
.
The encouraging news
Needless to say, we at Walking Tall have experienced a huge backlog of patients since being able to once again provide podiatric care on a more regular basis. To help with this, Anglicare set up a triage process to prioritise treatment, though this is slower than we would like (given COVID safe measures meant a reduction in the number of patients treated per day with the initial return of care and also skeleton staff being available).
The positive news
To end on a positive note, COVID ironically was the catalyst for some vast improvements in some of the more systemic issues surrounding homelessness. Australia provided shelters for 33,000 rough sleepers who were booked into hotels or other temporary accommodation. This has inspired several states to move beyond this phase and pledge similar support beyond COVID such as the Homes for Homelessness initiative in Victoria and the Together Home initiative in NSW.
The Queensland State Government provided funding for people who experienced homelessness during COVID’s peak; given they were unable to of course socially distance at home as requested. The funding provided an improvement in living conditions by offering hotel rooms to these people, and as long as each person adhered to standards set by the government around no drug use, keeping personal areas tidy and so forth, then they could reapply for seven days to continue and the health benefits were significant.
As a result of support like this, daily showers enabled an increase in hygiene and a decrease in bacteria and viral related infections and other health conditions that worsen with poor hygiene.
These developments demonstrate just how much intervention can make a difference in preventing or at least managing foot health (and wider health) issues in the homeless population. It will be interesting to watch this increasing intervention from state governments in this post COVID era when it arrives.
Say hello
Get in touch with the team at Walking Tall on Instagram or Facebook.