The changing labels of this condition
Children with generalised joint hypermobility (GJH) and related symptoms have been referred to within the literature under several different diagnostic labels, which have changed over time. Generalised joint hypermobility describes atypical high joint ranges of movement in multiple joints (Kirk, Ansell, & Bywaters, 1967) and presents in 20–40% of the paediatric population (Clinch et al., 2011; Remvig, Kümmel, Kristensen, Boas, & Juul-Kristensen, 2011) with approximately one-fifth of children with GJH reporting symptoms (Remvig et al., 2011; Sperotto et al., 2014).
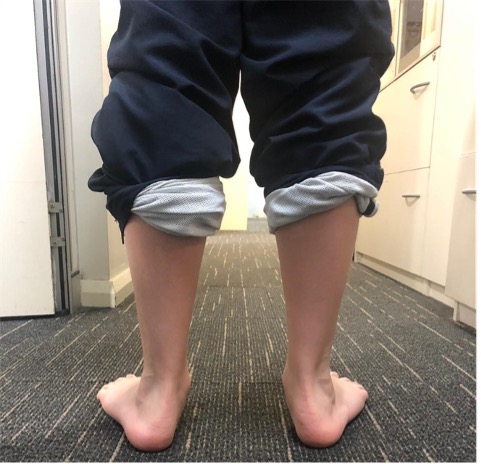
Figure 1: Posterior view of a child with GJH. consent obtained and photo provided by Narrabeen Sport Medical Centre – Podiatry.
Currently used diagnostic labels describing children with GJH with associated symptoms include Generalised Hypermobility Spectrum Disorder (G-HSD) (Castori et al., 2017), and hypermobile Ehlers-Danlos Syndrome (hEDS), which further incorporates an extended phenotype including skin involvement, tissue fragility or a marfanoid body habitus (excessively long limb) (Malfait et al., 2017). These conditions were previously referred to as Joint Hypermobility Syndrome (JHS) or EDS-Hypermobile type, with experts reporting a lack of clinical distinction between the two (Tofts, Elliott, Munns, Pacey, & Sillence, 2009) (Tinkle et al., 2009).
The term, ‘Children with GJH and associated symptoms’ will be used throughout this short article review to indicate any of the current or previously used terminology for this condition.
Going beyond hypermobility
Children with GJH and associated symptoms report chronic pain (Grahame, 2008), fatigue (Voermans, Knoop, Bleijenberg, & van Engelen, 2011) and functional difficulties, such as balance deficiencies (Hanewinkel-van Kleef, Helders, Takken, & Engelbert, 2009) that have a negative impact on their daily quality of life (Fatoye, Palmer, Macmillan, Rowe, & van der Linden, 2012) (Mu et al., 2019). Chronic joint pain is often exacerbated following physical activity (Armon, 2015) with lower limb pain being the most common location described (Pacey, Tofts, Adams, & Nicholson, 2015). Joint instability episodes and frequent soft tissue symptoms have also been frequently reported (Pacey et al., 2015); however, sometimes for young patients it is challenging to recollect with precision when and how these occurred.
Functional difficulties reported include motor development challenges (R. H. Engelbert et al., 2005), muscle torque deficits and poor proprioception (Fatoye, Palmer, Macmillan, Rowe, & van der Linden, 2009) resulting in a negative influence on school and/or social activity participation (Schubert-Hjalmarsson, Öhman, Kyllerman, & Beckung, 2012). Children with GJH also describe systemic symptoms including orthostatic intolerance, functional gastrointestinal disorders and stress incontinence (Fatoye et al., 2012; Pacey et al., 2015) a greater number of systemic symptoms leads to worse functional disability (Scheper et al., 2016).
Additional psychological symptoms may also result in poorer quality of life than typically developing children (Baeza-Velasco, Gély-Nargeot, Bulbena Vilarrasa, & Bravo, 2011; Mu et al., 2019; Pacey et al., 2015; Zekry, 2013)